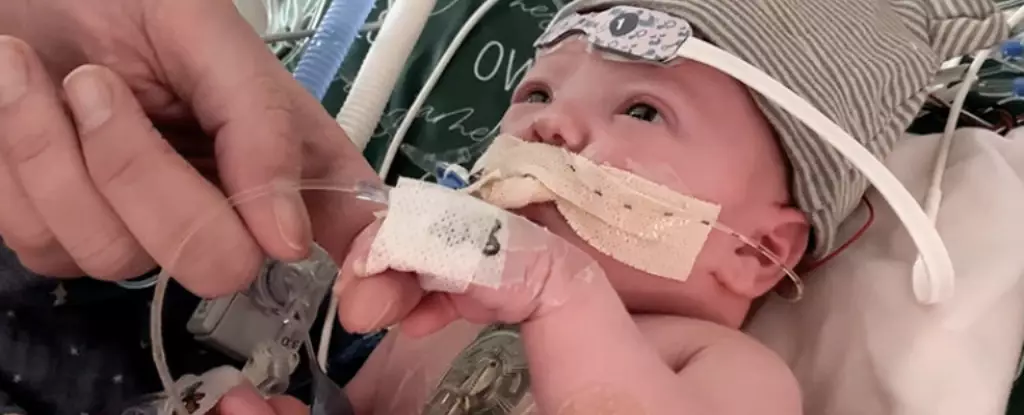
In a remarkable medical breakthrough, history was made in 2022 when surgeons performed the world’s first partial heart transplant in a baby. The recipient, Owen Monroe, who was just 18 days old at the time, underwent a groundbreaking procedure where heart valves and vessels taken from a donor infant were stitched into his heart. This innovative technique, which involved salvaging native heart tissue and replacing only the defective parts with donor tissue, had never been attempted in humans before. Spearheaded by the renowned surgeon, Joseph Turek of Duke University, this procedure had previously been successfully performed in piglets but had never been tested in humans.
Over a year later, the results of baby Owen’s partial heart transplant continue to exceed expectations. His implanted tissue has not only adapted to his growing body but has also undergone its own growth, exemplifying a phenomenon never witnessed in humans before. Owen’s heart, initially the size of a strawberry, has now expanded to the size of an apricot, demonstrating successful integration with his native heart tissue. Remarkably, Owen’s heart function is excellent, and he is achieving developmental milestones comparable to those of a typical one-year-old, such as playing, crawling, and standing. These extraordinary outcomes were reported in the Journal of the American Medical Association (JAMA) by the research team.
Baby Owen’s parents, Nick and Tayler Monroe, made the difficult decision to proceed with the surgery after learning of their son’s life-threatening heart defect known as truncus arteriosus. This condition, which affects approximately 250 babies in the US each year, occurs when a channel coming out of the heart fails to separate during development, resulting in the fusion of two major blood vessels and depriving the baby of oxygen. Traditionally, infants diagnosed with truncus arteriosus undergo a full heart transplant or receive frozen tissue from cadaver hearts.
While the hearts transplanted into infants do grow with them, they often become dysfunctional over time, leading to a high mortality rate. Shockingly, around 50 percent of children who receive a heart transplant will not survive beyond the age of 20. Moreover, to prevent the recipient’s body from rejecting the transplanted heart, immunosuppressive drugs are required. However, these drugs also suppress the immune system’s ability to fight infections and cancer, posing additional risks to the child’s health.
In Owen’s case, his partial transplant of vessels and valves only necessitated a reduced dosage of one immunosuppressive drug. This targeted approach minimizes the risk of rejection and alleviates the burden on his immune system compared to traditional heart transplant patients. Additionally, infants treated with frozen cadaver tissue for truncus arteriosus require multiple surgeries throughout their lives to replace the outgrown grafts. This poses a significant mortality risk of 50 percent during infancy, making the procedure highly risky.
Baby Owen’s journey to the partial heart transplant began with a sense of urgency. He was initially listed for a heart transplant, but due to the scarcity of suitable donor organs and the significant waiting time, his chances of survival were slim. Shortly after birth, Owen went into heart failure, rendering emergency treatments like extracorporeal membrane oxygenation (ECMO) ineffective due to his weakened heart. Faced with this critical situation, Owen’s parents felt that they had no alternative options.
Researchers and medical professionals involved in Owen’s case are hopeful that this groundbreaking procedure can be replicated in other children with similar conditions. The success of the partial heart transplant in Owen demonstrates the feasibility and potential of this technology in improving the lives of numerous children facing life-threatening heart defects.
The world’s first partial heart transplant in a baby has showcased unprecedented success and promises hope for a revolution in pediatric heart surgery. With further advancements and refined procedures, lives of countless infants afflicted with heart conditions like truncus arteriosus can be transformed. The triumph in Owen’s case paves the way for a new era in medical science, bringing solace and optimism to families facing seemingly insurmountable challenges.


Leave a Reply